Overview
One of the most common foot maladies people suffer from is plantar fasciitis. This condition arises when undue stress is placed on the ligament in your foot that supports your arch, the “plantar fascia”. When that ligament is overworked it leads to the classic symptoms of heel and arch pain which worsens when you get up to walk after periods of rest. This isn’t the kind of pain you experience after being on your feet all day at work or walking around Disneyland with your kids. The pain from plantar fasciitis is often intense and debilitating. It is also surprisingly common. Two million Americans suffer from plantar fasciitis every year and 10 percent of the population will experience it in their lifetime. It has become recognized as one of the most chronic and, often times, most difficult foot problems to treat.
Causes
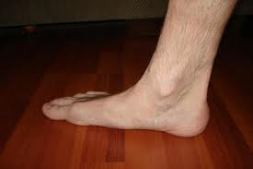
There are a number of possible causes for arch pain, but the most common are structural imbalances of the foot, such a pronated foot (rolls inward at the ankles). This is often not enough in isolation to cause the problem, but in combination with other factors arch pain may develop. These other factors are usually associated with overuse – running, walking, hard surfaces and/or OFAD (on feet all day), usually combined with inadequate or non-supportive footwear. The more common specific causes of arch pain can be plantar fasciitis (strain of the plantar fascia – a strong ligament that supports the arch), tarsal tunnel syndrome (a pinched nerve at the ankle that refers pain to the arch), foot strain from a pronated foot or flat foot, there can be osteoarthritis of the joints in the midfoot that can cause arch pain.
Symptoms
Symptoms of plantar fasciitis may occur anywhere along the arch, but it is most common near its attachment to the heel bone. Symptoms of plantar fasciitis vary, but the classic symptom is pain after rest–when you first get out of bed in the morning, or when you get up after sitting down for a while during the day. This is known as “post-static dyskinesia.” The pain usually diminishes after a few minutes of walking, sometimes even disappearing, but the pain is commonly felt again the longer you’re on the foot. Fasciitis can be aggravated by shoes that lack appropriate support, especially in the arch area, and by the chronic irritation of long-periods of standing, especially on concrete, and by being overweight. Other factors which influence this condition are gender (females get this more than men), age (30s to 50s are most common), and those with flatter-than-normal feet. It doesn’t help that fascia doesn’t heal particularly quickly. This is because it has relatively poor circulation, which is why it’s white in colour.
Diagnosis
After you describe your symptoms and discuss your concerns, your doctor will examine your foot. Your doctor will look for these signs. A high arch. An area of maximum tenderness on the bottom of your foot, just in front of your heel bone. Pain that gets worse when you flex your foot and the doctor pushes on the plantar fascia. The pain improves when you point your toes down. Limited “up” motion of your ankle.
Non Surgical Treatment
Treatment for a high arch foot or Charcot Marie Tooth disorder depends on the extent of deformity and the amount of disability experienced by the patient. Depending upon the symptoms, treatment may include. Changing the shoes. Special orthotic supports (devices that support, adjust, or accommodate the foot deformity). Cushioning pads. Foot and ankle braces or surgery.

Surgical Treatment
Although most patients with plantar fasciitis respond to non- surgical treatment, a small percentage of patients may require surgery. If, after several months of non-surgical treatment, you continue to have heel pain, surgery will be considered. Your foot and ankle surgeon will discuss the surgical options with you and determine which approach would be most beneficial. No matter what kind of treatment you undergo for plantar fasciitis, the underlying causes that led to this condition may remain. Therefore, you will need to continue with preventive measures. Wearing supportive shoes, stretching, and using custom orthotic devices are the mainstays of long-term treatment for plantar fasciitis.
Stretching Exercises
Achilles stretch. Stand with the ball of one foot on a stair. Reach for the step below with your heel until you feel a stretch in the arch of your foot. Hold this position for 15 to 30 seconds and then relax. Repeat 3 times. Balance and reach exercises. Stand next to a chair with your injured leg farther from the chair. The chair will provide support if you need it. Stand on the foot of your injured leg and bend your knee slightly. Try to raise the arch of this foot while keeping your big toe on the floor. Keep your foot in this position. With the hand that is farther away from the chair, reach forward in front of you by bending at the waist. Avoid bending your knee any more as you do this. Repeat this 15 times. To make the exercise more challenging, reach farther in front of you. Do 2 sets of 15. While keeping your arch raised, reach the hand that is farther away from the chair across your body toward the chair. The farther you reach, the more challenging the exercise. Do 2 sets of 15. Towel pickup. With your heel on the ground, pick up a towel with your toes. Release. Repeat 10 to 20 times. When this gets easy, add more resistance by placing a book or small weight on the towel. Resisted ankle plantar flexion. Sit with your injured leg stretched out in front of you. Loop the tubing around the ball of your foot. Hold the ends of the tubing with both hands. Gently press the ball of your foot down and point your toes, stretching the tubing. Return to the starting position. Do 2 sets of 15. Resisted ankle dorsiflexion. Tie a knot in one end of the elastic tubing and shut the knot in a door. Tie a loop in the other end of the tubing and put the foot on your injured side through the loop so that the tubing goes around the top of the foot. Sit facing the door with your injured leg straight out in front of you. Move away from the door until there is tension in the tubing. Keeping your leg straight, pull the top of your foot toward your body, stretching the tubing. Slowly return to the starting position. Do 2 sets of 15. Heel raise. Stand behind a chair or counter with both feet flat on the floor. Using the chair or counter as a support, rise up onto your toes and hold for 5 seconds. Then slowly lower yourself down without holding onto the support. (It’s OK to keep holding onto the support if you need to.) When this exercise becomes less painful, try doing this exercise while you are standing on the injured leg only. Repeat 15 times. Do 2 sets of 15. Rest 30 seconds between sets.
